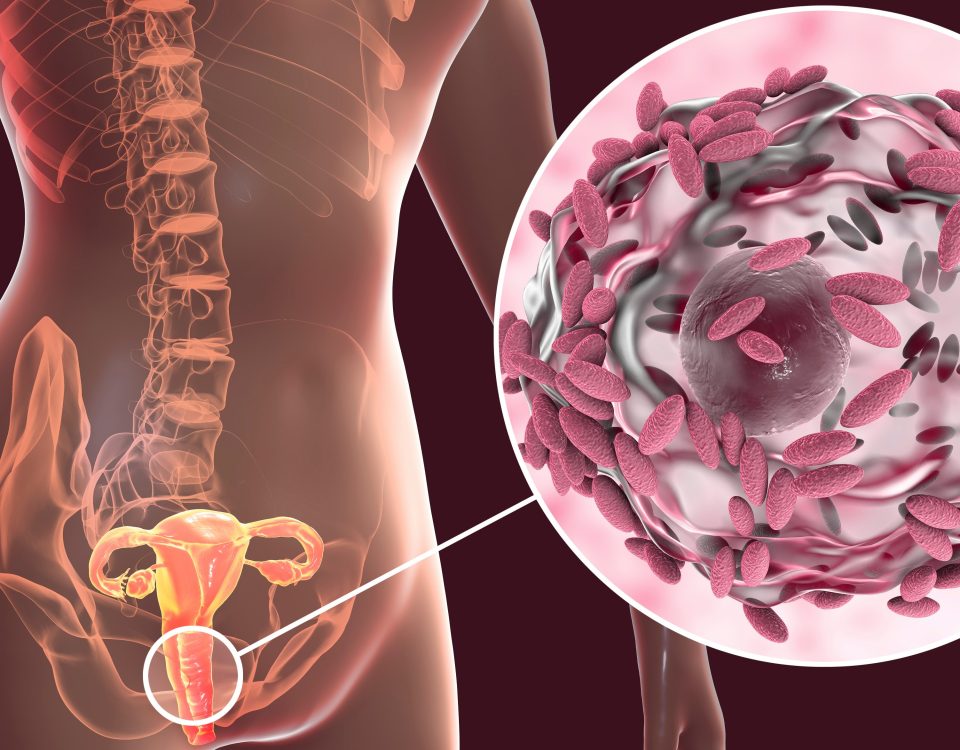
About one in five hospital patients in the United States have a urinary catheter, making it one of the most common indwelling devices among hospitalized patients1. A survey conducted by CDC in 20112 found that 45-79% of adult patients in critical care units have urinary catheters. Therefore, the use of urinary catheters is exceptionally prevalent in hospitals. Catheter-associated urinary tract infections (CAUTI), a form of Urinary Tract Infection (UTI), is the most commonly occurring health condition associated with the use of urinary catheters.
According to the CDC, about 75% of hospital-acquired UTIs are CAUTIs, and prolonged use of urinary catheters is associated with an increased risk of acquiring UTIs3. CAUTIs account for over 50% of hospital-acquired UTIs in long-term care facilities1. Every year, it is estimated that more than 1 million patients in healthcare facilities such as hospitals and nursing homes develop CAUTIs, and studies have shown that patients with CAUTIs have increased mortality and morbidity4.
Patients with chronic indwelling urinary catheters are typically assumed to have bacteriuria, and patients will receive antimicrobials as a standard of care. Although often asymptomatic, antimicrobial-resistant bacteria are commonly found in the urine of these patients1. However, the presence of uropathogens causes CAUTIs to develop, and CAUTIs can lead to other complications such as prostatitis, urinary catheter obstruction, bladder urolithiasis, endocarditis, meningitis, Etc.1,5
Study Detects Biofilms in Indwelling Catheters
A recent study published in the Journal of Urology showed that biofilms were detected within hours following catheter insertion6. An in-depth investigation into the location of biofilm formation confirmed that the catheter balloon and the lumen were primary locations of biofilm formation. Additionally, the researchers performed next-generation sequencing (NGS) on the biofilm samples.
The test results revealed that the biofilm is home to a variety of bacteria species. The most common bacteria include Enterococcus faecalis and Escherichia coli (E. coli). Other bacteria known to be uropathogenic such as Staphylococcus aureus and Staphylococcus epidermis, were also detected.
Most surprisingly, bacteria resistance genes were found to be present in almost half of the samples analyzed. The findings from this study highlight that uropathogens found growing in urinary catheters pose a significant public health concern, especially amongst hospitalized patients.
What are biofilms?
Biofilms are made of aggregates of micro-organisms and polymer matrices produced by the organisms that allow them to adhere to one another and surfaces. The matrices are typically composed of proteins, polysaccharides, and even nucleic acids. As such, biofilms are essential communities of micro-organisms that possess unique pro-survival characteristics such as social cooperation, resource capture, and enhanced survival of exposure to antimicrobials over free-floating microbes.7
Microbes within biofilms have been shown to be 10-10,000 times more antibiotic-resistant than free-floating ones.8 So why do biofilms thrive in urinary catheters? The environment created on the catheter surface promotes the formation of biofilms.
While the protective layers of matrices in biofilms help bacteria survive, they pose a significant medical problem simply because microbes in biofilms are difficult to diagnose and treat. Microbes in biofilms can also promote the formation of magnesium and calcium phosphate crystals that form a barrier to protect bacteria from antimicrobial compounds used to coat the catheters or circulating in patients.
The Usefulness of Next-Generation Sequencing DNA Diagnostics
With the health risks associated with CAUTI, especially amongst hospitalized patients, there is an imperative need for an accurate and comprehensive diagnostic tool that can identify microbes and pathogens in patients with CAUTIs. This is important in ensuring that the appropriate treatment is given to these patients.
As exemplified by the research study, next-generation sequencing is a powerful tool that can dissect out the microbial composition of biofilms. This is almost impossible to achieve using traditional urine culture techniques, which selectively favor the growth of a subset of microbes.
Also, pathogens that are present in small numbers will be outcompeted by other microbes that are present in larger numbers. Some microbes cannot be cultured using growth media. Therefore, NGS provides an unbiased approach to identifying and detecting microbes present in urine samples.
MicroGenDX’s NGS+qPCR Diagnostic Solution for Catheter-Associated UTIs
MicroGenDX, a leader in molecular diagnostics, offers an NGS+qPCR-based diagnostic solution for catheter-associated urinary tract infections. Within 3-5 days, MicroGenDX diagnostic test identifies the microbes present in a given sample. Additionally, MicroGenDX’s solution can detect 17 antibiotic resistance genes in 24-48 hours, giving physicians the ability to dispense the appropriate treatments, improving antibiotic stewardship and quality of care for patients with CAUTIs.
The two common misconceptions physicians have about NGS are that the turnover rates are lengthy and that the reports are too complicated. However, MicroGenDX has an average turnover time of 3.5 days, and there are resources provided to physicians who are new to the service.
CAUTI is a form of UTI that poses serious health threats, particularly among hospitalized patients who have urinary catheters. The is mainly due to the growth of biofilms on catheter surfaces which provides an optimal environment for microbes and pathogens to thrive. The presence of biofilms renders the diagnosis and treatment of these infections highly difficult.
The research study introduced earlier showed that biofilms were also found to harbor uropathogenic bacteria that could cause CAUTIs. Therefore, it is crucial to detect and identify microbes present in CAUTI patients using a comprehensive and accurate diagnostic tool. MicroGenDX’s qPCR+NGS will change how physicians approach CAUTIs. This will ultimately translate into more timely delivery of treatments to patients and higher quality patient care.
Resources
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4114799/
- https://www.cdc.gov/nhsn/PDFs/dataStat/NHSN-Report-2011-Data-Summary.pdf
- https://www.cdc.gov/hai/ca_uti/uti.html
- https://link.springer.com/article/10.1007/s00345-019-03071-4#ref-CR13
- https://www.cdc.gov/nhsn/pdfs/pscmanual/7psccauticurrent.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6952550/
- https://www.nature.com/articles/nrmicro.2016.94
- https://microgendx.com/next-generation-sequencing-helps-clinicians-win-the-war-against-biofilm-infections/